Everybody benefits from regular exercise.
If you have diabetes, or are at risk of diabetes, exercise plays an important role in keeping you health. The total amount of exercise should include a combination of aerobic and resistance training.
The benefits of exercise
There are so many great physical, mental and social benefits of exercise for people with Type 2 Diabetes.
- Improves cardiovascular health and fitness

- Decreases the risk of diabetes-related complications
- Improve physical function and independence
- Improves the blood supply and glucose delivery to muscles, resulting in effective use of energy from the diet
- Decreases risk of cardiovascular complications by improving risk factors such as high blood pressure and high cholesterol
- Helps manage and maintain effective blood glucose levels
- Decreases the doses of medications or insulin required
- Improves quality of life and mental health
- Increasing physical activity can reduce the incidence of T2DM by almost 60% in people at risk
Is exercise safe?
Exercise is important and benefical for everyone, but especially for people with Type 2 Diabetes. Finding the right exercise and being aware of the added considerations for exercise will ensure it’s both safe and effective. Consider the factors below to ensure exercise is safe:
- BGLs
- Medication
- Temperature
- Hydration
- Timing
Remember, if you have Diabetes complications (eg.retinopathy, nephropathy), other injuries or health conditions, you should talk to your doctor or an Accredited Exercise Physiologist before you start exercise. Our Exercise Physiologists have put together some tips and considerations for Starting Exercise with Type 2 Diabetes.
Who should exercise?
Although some risks are associated with physical activity for people with T2DM, the risks of inactivity mostly outweigh them. The following points should be kept in mind before starting an exercise program:
Low blood glucose: If necessary, consult with your health professional before commencing exercise to discuss your medications and monitoring of your blood glucose levels. Exercise may need to be temporarily modified.
Risk of cardiac events (e.g. heart attacks). People wishing to exercise vigorously, older people, and people with established cardiovascular disease should be screened prior to commencement of their program;
Peripheral neuropathy. Appropriate footwear, regular foot inspection and low-impact exercises are essential with peripheral neuropathy, and are also highly advised for all people with T2DM;
Hypertension (high blood pressure). Although exercise reduces hypertension, those with poorly controlled blood pressure should avoid vigorous exercise, particularly resistance training of vigorous intensity;
Obesity. For overweight people with T2DM, weight loss will reduce joint pain and discomfort when exercising, and encourage them to continue exercising.ink to Exercise Physiology
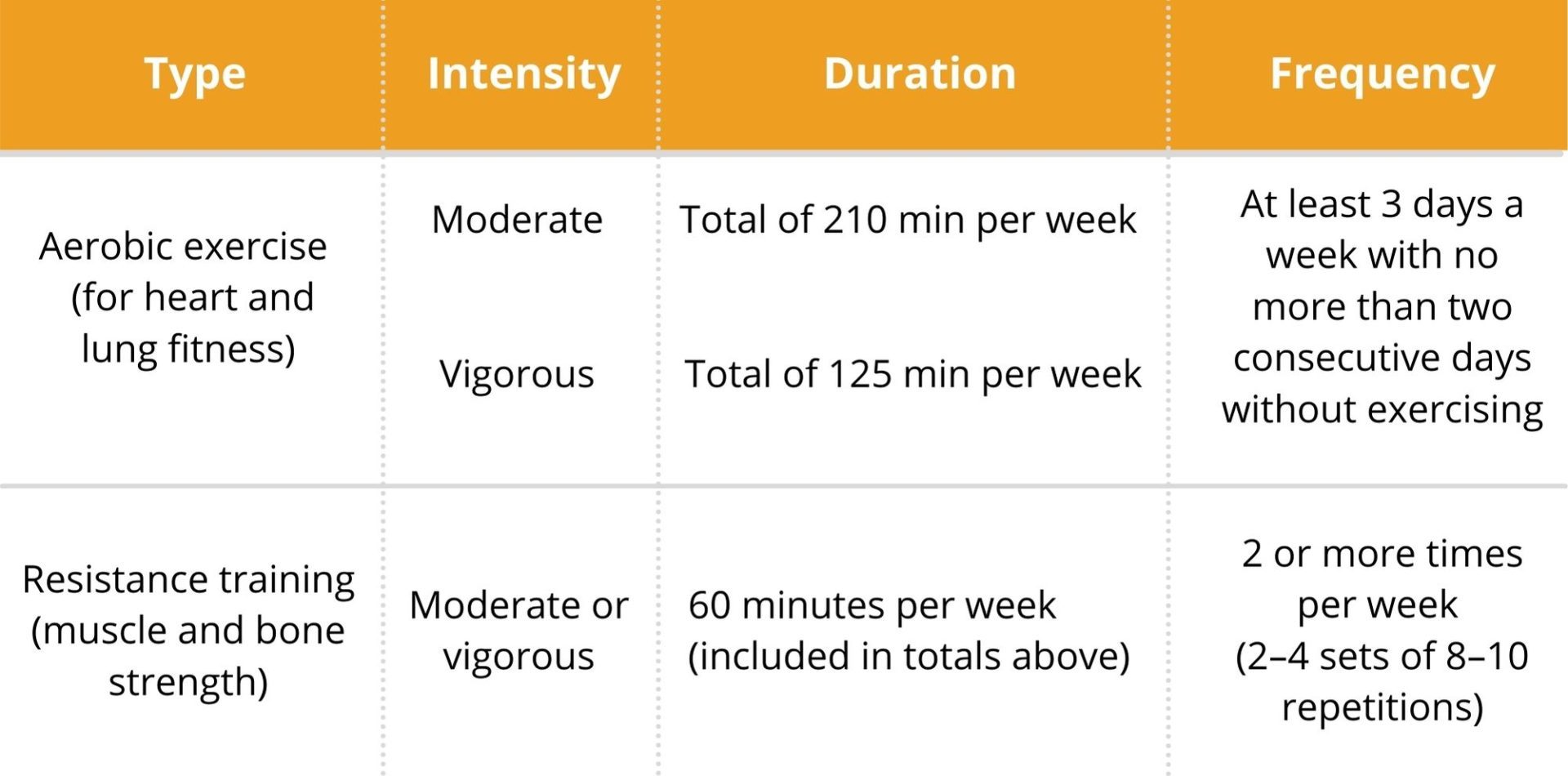
What type of exercise
The table above shows the type, intensity, duration and frequency of exercise recommended for people with T2DM and should be the goal to work towards. Check out our Tips for Starting Exercise and remember to focus on progress over perfection!
Resistance Training
Resistance training is a type of exercise performed using resistance to build strength, anaerobic endurance and size of skeletal muscle. Often the resistance comes from using weights, but depending on your capacity and goals, it may also include bodyweight exercises or use of resistance bands.

Benefits
- Provides an initial post-exercise blood glucose decline with prolonged reductions over next 24hr (compared to engaging in aerobic exercise only).
- Effective at increasing lean muscle mass (hypertrophy), strength and power to improve body composition (reduce body fat)
- Increasing lean muscle mass improves insulin sensitivity and reduces HbA1c and blood glucose levels
- Improves functional balance and risk of falls
- Reduces decline in muscle atrophy from deconditioning
How much?
- 60 minutes OR 2 or more 30mins sessions per week
- 2–4 sets of 8–12 repetitions
- Progressive resistance training targeting major muscle groups and accessory muscles to gain greatest benefits.
- A program which is tailored to individual health concerns and lifestyle choices.
- Pilates and Yoga compliments resistance exercise as it involves bodyweight strength and stability, but should not replace weighted training.
Aerobic Training
Aerobic exercise is also called cardiovascular training or cardio. “Aerobic” means “with oxygen” and refers to the use of oxygen to provide fuel to the muscles during exercise. The rise in breathing and heart rate during exercise is to increase the rate of oxygen delivery. Over time, aerobic training can increase the efficiency of oxygen delivery and consumption and result in improved cardiovascular fitness.

Benefits
- Increases cardiorespiratory fitness
- Increases glucose uptake from the blood to reduce insulin resistance or need for medication.
- Reduces circulatory lipids to improve cholesterol levels, blood vessel function and heart health.
- Improves blood vessel dilation and circulation which results in improved blood pressure levels.
How much?
- Aim to be physically active on most days of the week.
- 210 moderate intensity mins/week or 125 vigorous intensity min/week
- It is recommended to engage in consistent exercise that is spread out over the week rather than completing it all in one day then not again for another week.
- Aerobic training examples: walking, cycling, running, swimming, dancing, water aerobics, social sport/activities etc.
- People with Diabetes should discuss exercise with a health professional before starting to address additional safety considerations.
Not sure where to start? Link to Exercise Physiologist or Download our 4 week Physical Activity planner to
