Ovarian cancer is the eighth most common type of cancer for women in Australia, with more than 1500 women diagnosed each year.
Despite being less common than other female cancers, the absence of an early detection test and difficulty in recognising and diagnosing symptoms, means that ovarian cancer has the highest mortality rate of all gynaecological cancers. Ovarian cancer is predominantly diagnosed in women over the age of 50 (the average age of diagnosis is 64) but it can occur in younger women.
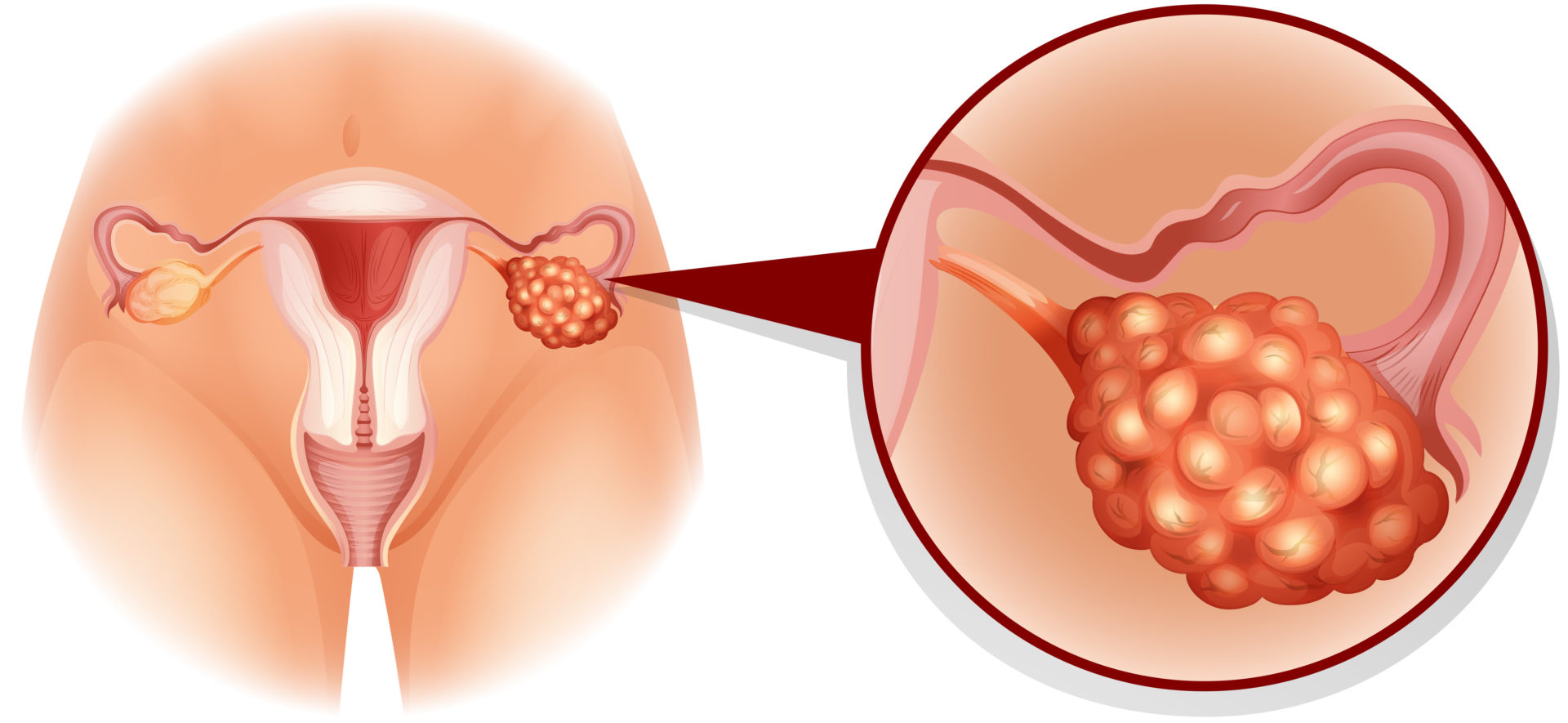
Risk Factors, Signs and Symptoms
The exact causes of most ovarian cancers are unknown, however, there are factors that may increase a woman’s risk of developing ovarian cancer.
Increasing age is the biggest risk factor and while ovarian cancer can happen at any age, it usually occurs in women who have been through menopause. Hereditary factors also account for approximately 20% of ovarian cancers.
Other factors that may increase the risk of ovarian cancer include:
- having endometriosis
- a previous breast cancer diagnosis
- having diabetes
- being overweight
- smoking
- not having had children
Symptoms for ovarian cancer can be vague and are often difficult to diagnose because many can be caused by other less serious medical conditions. The most reported symptoms for ovarian cancer are:
- Increased abdominal size or persistent abdominal bloating
- Abdominal or pelvic (lower tummy) pain
- Feeling full after eating a small amount
- Needing to urinate often or urgently
Additional Symptoms may include:
- Changes in bowel habits
- Unexplained weight gain or loss
- Excessive fatigue
- Lower back pain
- Indigestion or nausea
- Bleeding after menopause or in-between periods
- Pain during sex or bleeding after
Treatment & Side Effects
An individual treatment plan is developed, depending on the type and stage of ovarian cancer, general health, and other personal factors such as the desire to have children in the future.

Most women with ovarian cancer will need surgery and for early-stage ovarian cancers, this is usually the only treatment necessary. For more advanced ovarian cancer, chemotherapy may be used in combination with surgery, to shrink the size of the tumour or to stop the cancer coming back. Other treatments that are used to treat ovarian cancer are radiotherapy and biological therapies.
Throughout treatment, women often report a variety of side effects such as fatigue, peripheral neuropathy (tingling, burning or numbness), hair and skin issues, and psychological distress.
The surgery, chemotherapy and radiotherapy used to treat ovarian cancer can cause ‘early menopause’ in women who have not yet reached natural menopause. Differing from the gradual transition of natural menopause, early menopause from cancer treatment is a far more sudden drop in hormones. The changes that result from this hormone drop are different for everyone: some women may not have troublesome symptoms at all, while for others, symptoms can greatly affect them.
Common and troublesome symptoms include:
- hot flushes and sweats
- sleep disturbances (insomnia)
- vaginal dryness
- lowered libido (sex drive)
- changes in mood (sadness, depression, and anxiety)
Exercise and Ovarian Cancer
Exercise plays a vital role before, during and after ovarian cancer treatment. There is well established evidence that exercise can not only reduce the incidence and severity of treatment side effects, but it can also reduce the risk of recurrence. Exercise is also able to improve or maintain functional capacity during and after treatment, reduce the risk of developing other chronic diseases and have better overall survival.

Fatigue One of the most reported side effects of cancer treatment is cancer-related or post-cancer fatigue. Exercise is the first-line therapy for managing cancer-related fatigue and is more effective than medication or rest.
Mental Health Exercise can have benefits well beyond the physical. Women affected by ovarian cancer often report distress and depressive symptoms. Exercise has established benefits for managing mental and emotional health, reducing symptoms of depression and anxiety, and can restore a sense of control and confidence once again.
Peripheral Neuropathy Increasing movement and heart rate can help in the prevention and management of peripheral neuropathy. Physical activity can improve blood circulation, which strengthens nerve tissues by increasing the flow of oxygen and can reduce associated pain. Balance training can also reduce the impacts of peripheral neuropathy on impaired balance.
Menopause Specific physical activity, including cardiovascular based exercise, can assist in managing symptoms including hot flushes, night sweats, mood, and sleep disturbances. Post menopause, there is a higher incidence of cardiac conditions and osteoporosis, but the risk factors for these conditions can be managed with specific types of exercise.
Exercise Right
The Clinical Oncology Society of Australia advises exercise is a safe, effective, and a necessary part of cancer treatment for all cancer types. They recommend a tailored exercise program from an accredited exercise physiologist for those undergoing treatment and in recovery from ovarian cancer. They suggest that patients work towards the exercise guidelines for both aerobic and strength-based exercise, achieving 150-300 minutes of moderate intensity exercise and two strength-based sessions per week. Both during treatment and recovery, it is important to progress towards this amount of exercise gradually and safely.
How can an Accredited Exercise Physiologist help?
An Accredited Exercise Physiologist (AEP) is an allied health professional, trained to prescribe exercise as medicine, ensuring safety and maximising therapeutic benefits. An AEP who specialises in Exercise Oncology has an additional training in cancer care and has comprehensive knowledge of the phases of a cancer diagnosis, cancer treatments and their side-effects, and how to prescribe and adapt exercise at all stages of the cancer care continuum.

As each woman experiences ovarian cancer differently, the exercise program will always be tailored to the needs of the individual, allowing for adjustment and modification at every stage throughout and beyond treatment. As allied health professionals, an AEP will work alongside other health providers to ensure the best holistic care.
An AEP will talk to you about your cancer, your treatment pathway, current or potential side-effects and assess your physical capacity. Using this information, your medical history, personal goals, preferences and lifestyle factors, your AEP can determine the most appropriate “dose” of exercise for you.
Find out more about Bodytrack’s Cancer Care Services or meet our Exercise Oncology Specialists Caitlin and Nicole.
